What is prostatitis? We will analyze the causes of occurrence, diagnosis and methods of treatment in the article of a doctor, urologist with 28 years of experience.
Definition of disease. Causes of the disease
ProstatitisIs an inflammatory process of the prostate tissue, accompanied by pain in the lower back, perineum or pelvic region, as well as disturbances in the work of the lower urinary tract.
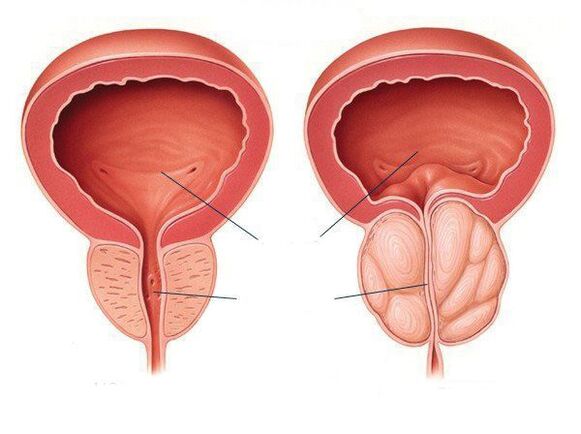
The prostate (prostate) refers to the male reproductive system. It sits in front of the rectum, below the bladder, and surrounds the urethra (urethra). That is why, when the prostate becomes inflamed, it compresses the urethra, which further leads to various urination problems. The main function of the prostate is the production of secretion (fluid), which is part of semen and liquefies it to ensure normal sperm motility.
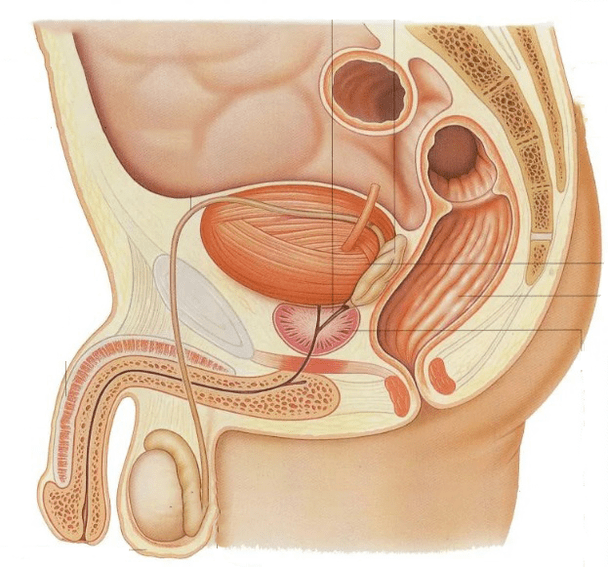
Pathological conditions of the prostate, such as cancer or benign hyperplasia, are more common in older patients. Prostatitis differs in that it affects men of all age groups, but most often the disease occurs in men of childbearing age (8-35% of cases).
Prostatitis most often occurs in the practice of a urologist. It can occur suddenly (acute) or gradually, and its manifestations are constant and long-term (chronic). The chronic form is much more common than the acute form. Chronic prostatitis ranks fifth among twenty major urologic diagnoses.
Prostatitis can either be an independent disease or be associated with benign prostatic hyperplasia and prostate cancer. In recent years, there has been a decrease in the incidence of prostatitis in the male population: if in 2012 the incidence was 275 per 100, 000 of the population, then in 2017 the primary incidence was 203 per100, 000 of the population.
The reasons for the development of prostatitisare bacterial (infectious) and non-bacterial (non-infectious).Infectious prostatitismore common in men under 35. Most often, this form of the disease is caused by Gram-negative microorganisms, in particular Enterobacter, E. coli, serrations, pseudomonas and proteus, as well as sexually transmitted infections, such as gonococcus, chlamydia, etc. Very rarely, prostatitis can occur due to Mycobacterium tuberculosis. In chronic bacterial prostatitis, the spectrum of pathogens is broader and may include atypical pathogens. It should be remembered that chronic bacterial prostatitis is a polyetiological disease, that is, it can have several causes.
Factors contributing to the development of inflammationin the prostate:
- sexually transmitted infections;
- immunodeficiency states;
- prostate biopsy;
- invasive manipulations and operations;
- Way of life;
- diarrhea, constipation;
- homosexual contact;
- frequent change of sexual partners;
- sedentary lifestyle, etc.
Chronic non-bacterial prostatitisdiagnosed in patients who complain of chronic pain in the prostate area, while no infectious (bacterial) agent of the disease has been found in them. Despite numerous studies, the cause of this type of chronic prostatitis is not fully understood, however, some factors can cause its development:
- increased prostate pressure;
- muscle pain in the pelvic area;
- emotional disturbances;
- Autoimmune disorders (antibodies that are supposed to fight infection, sometimes for some reason attack prostate cells);
- physical activity;
- irregular sex life;
- lifting weights, etc.
In some cases, prostatitis can occur after performing transurethral procedures such as urethral catheterization or cystoscopy, as well as after a transrectal biopsy of the prostate.
Although the actual incidence of various types of prostatitis has not been definitively established, the following data is provided:
- acute bacterial prostatitis accounts for about 5-10% of all prostatitis cases;
- chronic bacterial prostatitis - 6-10%;
- Chronic non-bacterial prostatitis - 80-90%;
- prostatitis, including prostatodynia (neurovegetative disorders of the prostate) - 20-30%.
If you notice similar symptoms, see your doctor. Don't self-medicate - it's dangerous for your health!
Symptoms of prostatitis
All forms of inflammationthe prostate, in addition to the asymptomatic, is united by the presence of the following symptoms:
- pain in the lumbar region;
- feelings of discomfort with intestinal peristalsis;
- pain in the perineum or pelvic area;
- disturbances in the work of the lower urinary tract.
The main symptoms of the lower urinary tract in the presence of prostatitis:
- frequent urge to urinate;
- difficulty urinating, that is, weak flow and the need to "filter";
- burning pain or its intensification when urinating.
In diagnosed menacute bacterial prostatitisPelvic pain and urinary tract symptoms such as increased urination and urinary retention occur. This can lead to the development of systemic manifestations such as fever, chills, nausea, vomiting and malaise. Acute bacterial prostatitis is characterized by an abrupt onset of the disease with a vivid clinical picture. It is a serious illness.
Men diagnosedchronic bacterial prostatitisnote symptoms of a periodic nature, which increase and decrease. With an exacerbation, pain and discomfort are noted. Pain sensations are localized mainly at the base of the penis, around or above the anus. Also, the pain can occur just above the pubic bone or in the lower back, spreading to the penis and testicles. Defecation also becomes painful. Sometimes signs of infection of the lower parts of the urinary system develop: burning pain and frequent urination, frequent urge. These symptoms can be confused with the manifestations of acute bacterial prostatitis, but it usually manifests itself as a sudden onset, chills, fever, weakness, pain throughout the body, in the lower back, as well asin the genitals, frequent painful urination, pain with ejaculation. If you notice such symptoms, you should seek urgent medical attention.
If the modern standard examination has not established that chronic pain is caused by a pathological process in the prostate, then we are dealing with chronic non-bacterial prostatitis, also calledchronic pelvic pain syndrome(the term has been used since 2003). In the presence of chronic pelvic pain syndrome, a man's quality of life is significantly reduced, as this syndrome sometimes leads to various psychological and sexual disorders:
- increased fatigue;
- feeling helpless;
- erectile dysfunction;
- painful ejaculation;
- pain after sex, etc.
In chronic non-bacterial prostatitis / chronic pelvic pain syndrome, there is a feeling of discomfort or persistent pain in the lower back, most often at the base of the penis and around the anus, for at least 3 months. Painful sensations are localized in a "target organ" or several pelvic organs. Most often, with this form of prostatitis, the pain is localized in the prostate (46%).
In chronic prostatitis, sexual disorders exhibit a number of characteristics. First, all components of a man's copulative (sexual) function are disturbed to varying degrees: libido, erection, ejaculation. Second, sexual dysfunction mainly occurs in people with a long history (more than 5 years) of the disease. Third, sexual dysfunction is often the main reason for seeing a doctor.
Erectile dysfunction is noted by 30% of patients with chronic prostatitis, largely due to the psychogenic factor - a catastrophic perception of the disease.
Symptoms of prostatitis occur at least once in a lifetime in 50% of men.
Pathogenesis of prostatitis
The mechanism of development of prostatitis is multifaceted and very complex. Many factors are involved in its development. Most cases of acute bacterial prostatitis are caused by a cascade of processes triggered by ascending urethral infection or intraprostatic reflux (reflux of urine).
The penetration of microorganisms into the prostate is possible ascending (through the urethra) or transrectally through the lymphatic route. Diarrhea and constipation associated with impaired rectal barrier function are considered to be a provoking factor in chronic prostatitis. However, the mechanism of penetration of microorganisms into the prostate is still not clearly established.
Urinary disorders with prostatitis can result from:
- increase the tone of smooth muscles of the prostatic urethra by increasing the activity of adrenergic receptors;
- enlarged prostate or narrowing of the urethra, resulting in turbulent urine flow, obstruction of the bladder outlet, and intraprostatic reflux.
In the future, there is a violation of the drainage of the prostate ducts, stagnation of secretions from the prostate, edema, activation of the arachidonic acid cascade, inflammation and ischemia. A vicious circle of pathological changes is formed.
Classification and stages of development of prostatitis
There are 4 main categories (types) of prostatitis.
- Acute bacterial prostatitis(category I).
- Chronic bacterial prostatitis(category II).
- Prostatitis / chronic non-bacterial syndromechronic pelvic pain (category III). May be inflammatory (category III A) or non-inflammatory (category III B).
- Asymptomatic inflammatory prostatitis.Histological prostatitis identified by prostate biopsy (category IV).
Chronic bacterial prostatitiscontrary tospice,is manifested by recurrent episodes of exacerbation with the presence or absence of complete remissions between them. Symptoms are generally less severe than those of acute prostatitis.
Classification of the National American Institutes of Health. . .
- Type I(acute bacterial prostatitis) - acute infection of the prostate: symptoms of the disease appear suddenly. Chills, fever, pain all over the body, weakness, pain in the lower back and genital area, frequent painful urination, pain when ejaculation. Potential symptoms of acute bacterial prostatitis include blood in the urine and / or semen. It's rare. It is being treated effectively with antibiotics.
- type II(chronic bacterial prostatitis) - a chronic or recurrent infection of the prostate: the symptoms are the same as in acute prostatitis, but appear gradually and are less pronounced. Several courses of antibiotic therapy may be necessary.
- III type(chronic non-bacterial prostatitis and chronic pelvic pain syndrome): no signs of infection.
- III A type: presence of leukocytes in the ejaculate / prostatic secretion / third portion of urine obtained after massage of the prostate.
- Type IIIB: absence of leukocytes in the ejaculate / prostatic secretion / third portion of urine obtained after massage of the prostate. Pain in the lower back and genital area, frequent urination, difficulty urinating (often at night), burning or painful urination, and ejaculation. Account for about 90% of all cases of prostatitis. There are no known causes or clinically proven treatments.
- type IV(asymptomatic inflammatory prostatitis): Sometimes an increase in the number of white blood cells. No treatment required. Detected on prostate biopsy.
The boundaries between the different forms of prostatitis are blurred.
Complications of prostatitis
With inflammatory lesions of the prostate, neighboring organs are involved in the pathological process: the seminal tubercle, Cooper's glands, seminal vesicles and the posterior urethra. The infection can simultaneously enter the prostate and surrounding organs.
Vesiculitis- inflammation of the seminal vesicles. The pain is localized in the groin area and deep in the pelvis, radiating to the sacrum. The pain is usually one-sided, as both seminal vesicles are affected to varying degrees. Vesiculitis can be asymptomatic. The only complaint from patients may be the presence of blood in the semen. Periodic pyuria (pus in the urine) and pyospermia (pus in the ejaculate) are also noted.
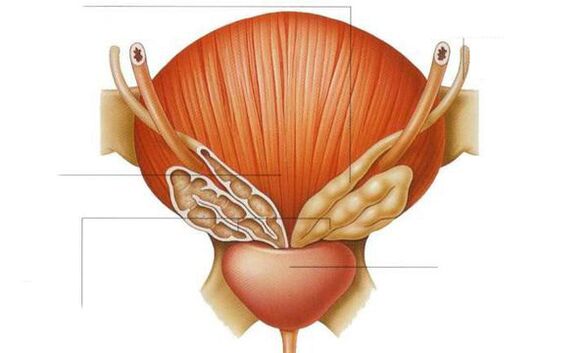
Posterior urethritis, colliculitis (inflammation of the seminal tubercle). . . With prostatitis, the infection enters the seminal tubercle, this is due to the proximity of the prostate to the excretory ducts.
Prostate abscess.Pathogens that cause prostatitis can also cause prostate abscess. It is a serious septic (bacterial) disease, which is accompanied by weakness, fever, chills with profuse sweat. In some cases, altered consciousness and delirium are observed. The patient needs to be hospitalized.
Sclerosis of the prostate (fibrosis).This is a late complication of prostatitis, which is based on the replacement of prostate tissue with scarring (connective tissue degeneration, that is, sclerosis), which leads to the fact that the gland shrinks, decreases in size and completely loses its function. As a rule, sclerotic symptoms develop long after the onset of the inflammatory process in the prostate.
Prostate cysts.These formations can contribute to the formation of stones in the prostate. The presence of an infection in a cyst can lead to an abscess of the prostate. It is not difficult to diagnose a prostate cyst using ultrasound. They can also be detected by a digital rectal exam.
Prostate stones.They are quite common. The causes of the disease are not fully understood, but most experts agree that they are the result of a prolonged inflammatory process in the prostate. The stones are simple and multiple, with a diameter of 1 to 4 mm. Large stones are rare. The stones clog the gland, because of which the secret stagnates there, the gland is stretched too far and separate cysts are formed, into which the infection enters. Patients with stones in the prostate have to deal with constant dull pain in the perineum. The painful sensations spread to the glans and cause frequent urges to urinate, which becomes difficult and painful.
Infertility.Long-term chronic prostatitis primarily reduces the motor function of sperm, making them completely immobile. One of the consequences is a violation of their production, the formation of immature sperm that have an abnormally altered shape (and a smaller number than before).
Ejaculation disorder.Prostatitis in all its forms causes sexual dysfunction. At first, patients are faced with premature ejaculation, have a normal erection, which subsequently weakens, and the degree of orgasm decreases. The prolonged existence of chronic prostatitis contributes to a decrease in the production of male sex hormones and a weakened libido.
Dyserection.The relationship between chronic prostatitis / chronic pelvic pain syndrome and erectile dysfunction has been described. This disorder is particularly painful for men.
Diagnosis of prostatitis
The appearance of the first signs of inflammation of the prostate requires immediate medical attention. The urologist will exclude many diseases with similar manifestations and determine to which category (type) the disease belongs. Before choosing a treatment, a specialist will carry out the necessary examinations and offer to undergo an evaluation test.
What questions might the doctor ask
During the appointment, the doctor will definitively specify: the duration of the clinical manifestations of the disease, the location and the nature of the pain, for example in the perineum, the scrotum, the penis and the inside of the thigh; changes in the nature of the semen (presence of pus and blood).
At the reception, the urologist will offer to fill out special questionnaires, one of them is the index of symptoms of chronic prostatitis.
The patient should ask the doctor questionswhat tests and studies will need to be done, how to prepare for them, what treatment he plans to prescribe and where I can get more information about the disease.
Chronic bacterial prostatitis is diagnosed when symptoms last for at least three months.
The investigation will include:
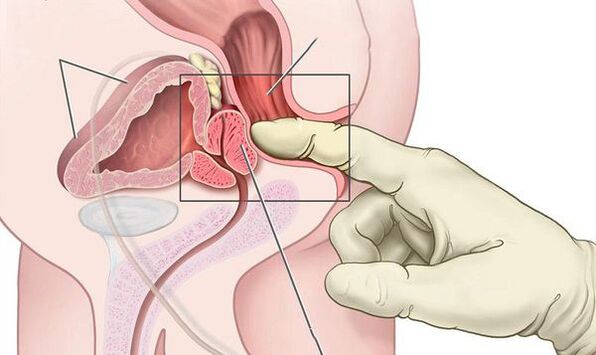
- Digital rectal examination of the gland to determine the extent of the enlarged prostate and its consistency.
- Tests for secretions from the prostate, urine and / or ejaculate.
- Identification of urogenital infection.
- Ultrasound examination of the urinary system (kidneys, prostate, bladder with determination of residual urine).
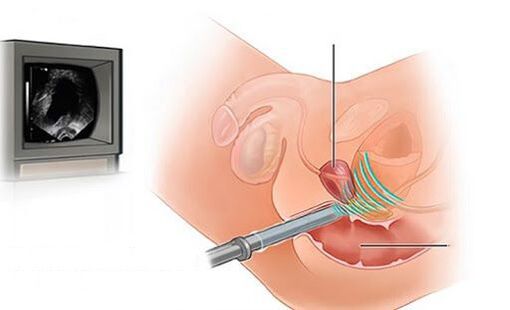
- Urodynamic study.
In the case of acute bacterial prostatitis, a swollen and painful prostate can be found with a digital rectal exam. Prostate massage is contraindicated because it can lead to bacteremia and sepsis.
The most important study in the examination of patients with acute bacterial prostatitis is the culture of prostatic secretions. In order to categorize chronic prostatitis, quantitative culture and microscopy of urine samples and prostatic secretions obtained after prostate massage remain important methods.
Androflor - a comprehensive study of the microbiocenosis of the urogenital tract in humans by PCR. Allows to determine the qualitative and quantitative composition of the microflora. It is used to diagnose and monitor the treatment of inflammatory infectious diseases of the genitourinary system.
After identifying the cause of the disease, the doctor will recommend treatment. It should be remembered that standard methods can detect infection only in 5-10% of cases, which ultimately leads to prostatitis.
What is the Relationship Between Prostatitis, Prostate Specific Antigen (PSA), and Prostate Cancer
Measurement of total and free PSA levels in prostatitis does not provide additional diagnostic information. It is known that in 60 and 20% of patients with acute and chronic bacterial prostatitis, the level of prostate specific antigen (PSA), respectively, increases. After the end of treatment, the PSA level decreases in 40% of patients. PSA is not considered to be a specific marker for prostate cancer because PSA levels can be elevated in benign prostatic hyperplasia and prostatitis.
Treatment of prostatitis
The main role in the treatment of pathology is assigned to pharmacotherapy.
Alpha1-blocker therapy
Alpha1-blockers are prescribed to patients who complain of difficulty in passing urine. These drugs help make urination easier and relax the muscles of the prostate and bladder. Some patients are prescribed drugs to lower hormone levels, which can help shrink the gland and reduce discomfort. Muscle relaxants can help relieve pain caused by an edematous prostate that puts pressure on nearby muscles. Nonsteroidal anti-inflammatory drugs (NSAIDs) can help with pain.
Standard antibiotic therapy in most cases does not lead to a decrease in the number of relapses of the disease, and therefore an integrated approach is often used and is also prescribedancillary drugs: biostimulants, extracts from various plants and insects and their biological components, which may be in the formrectal suppositories. . . Despite the large arsenal of drugs, the effectiveness of their use remains insufficient.
Physiotherapy in the treatment of prostatitis
For chronic prostatitis of categories II, III A and III B, physiotherapeutic methods can also be used:
- prostate massage (prostate);
- laser therapy;
- microwave hyperthermia and thermotherapy;
- electrical stimulation with modulated currents of skin or rectal electrodes;
- acupuncture (acupuncture).
The efficacy and safety of these treatments are still under investigation. Also used for the treatment of prostatitisfolk methods, for examplehirudotherapy.The efficacy and safety of this method for the treatment of prostatitis has not been proven.
Injection of stem cells
Cell therapy (stem cell injections) in the treatment of prostatitis is currently a promising technique in the early stages of development. At the moment, regarding the injection of stem cells into the prostate, we can only have hypotheses about its mechanisms, as well as empirical data obtained by groups of individual researchers.
Surgical treatment of prostatitis
Surgical methods are used only to treat complications of prostatitis - abscess and suppuration of the seminal vesicles.
Treatment of chronic pelvic pain syndrome requires a separate examination. Asymptomatic inflammatory prostatitis (grade IV) should not be treated unless the patient is considering prostate surgery. In this case, the patient is given prophylactic antibiotics.
Diet and lifestyle for prostatitis
A special diet for prostatitis is not necessary, but eating plenty of vegetables, lean meat, and dairy products will improve bowel function. It is important to consume enough fiber, foods rich in vitamin E (wheat germ, corn oil, etc. ), sugar should be replaced with natural honey. Proper nutrition for prostatitis can improve bowel function and reduce the likelihood of relapse or speed up recovery. It is recommended that you adopt a healthy lifestyle, drink more fluids, and limit caffeine and alcohol.
Provide. Prophylaxis
Acute prostatitis often becomes chronic, even with timely and adequate treatment.
Full recovery is not always possible, however, with correct and constant treatment and following the doctor's recommendations, it is possible to eliminate discomfort and pain. Independenttreatment of prostatitis at homecan be dangerous and cause complications.
Not all cases of prostatitis can be identified as a cause, but there are a number of steps you can take to try and prevent prostatitis. The same steps can help control existing symptoms:
- Drink lots of fluids. Drinking a lot of fluids causes frequent urination, thus facilitating the evacuation of infectious agents from the prostatic urethra.
- Empty your bladder regularly.
- Avoid irritation of the urethra. Limit your intake of caffeine, spicy foods, and alcohol.
- Reduce pressure on the prostate. Men who cycle often need to use a split seat to relieve pressure on the prostate.
- Stay sexually active.



























